Ask A Neuroscientist: Cannabis and Sleep
Neurobiological Mechanisms, Therapeutic Potential, and Clinical Considerations
Cannabis is one of the most widely used sleep aids in the world — but the science behind how it works is far more complicated than “it makes you drowsy.” Depending on which compounds are in it, how much you use, when you use it, and your own biology, cannabis can help you fall asleep faster, suppress dreaming, disrupt your sleep cycles, or make your sleep worse over time. This article breaks down what the research actually shows: how cannabis interacts with your brain’s sleep systems, what THC, CBD, and CBN each do at different doses, and what heavy or long-term use can mean for your sleep health.The Cannabis-Sleep Relationship: Beyond Simple Sedation
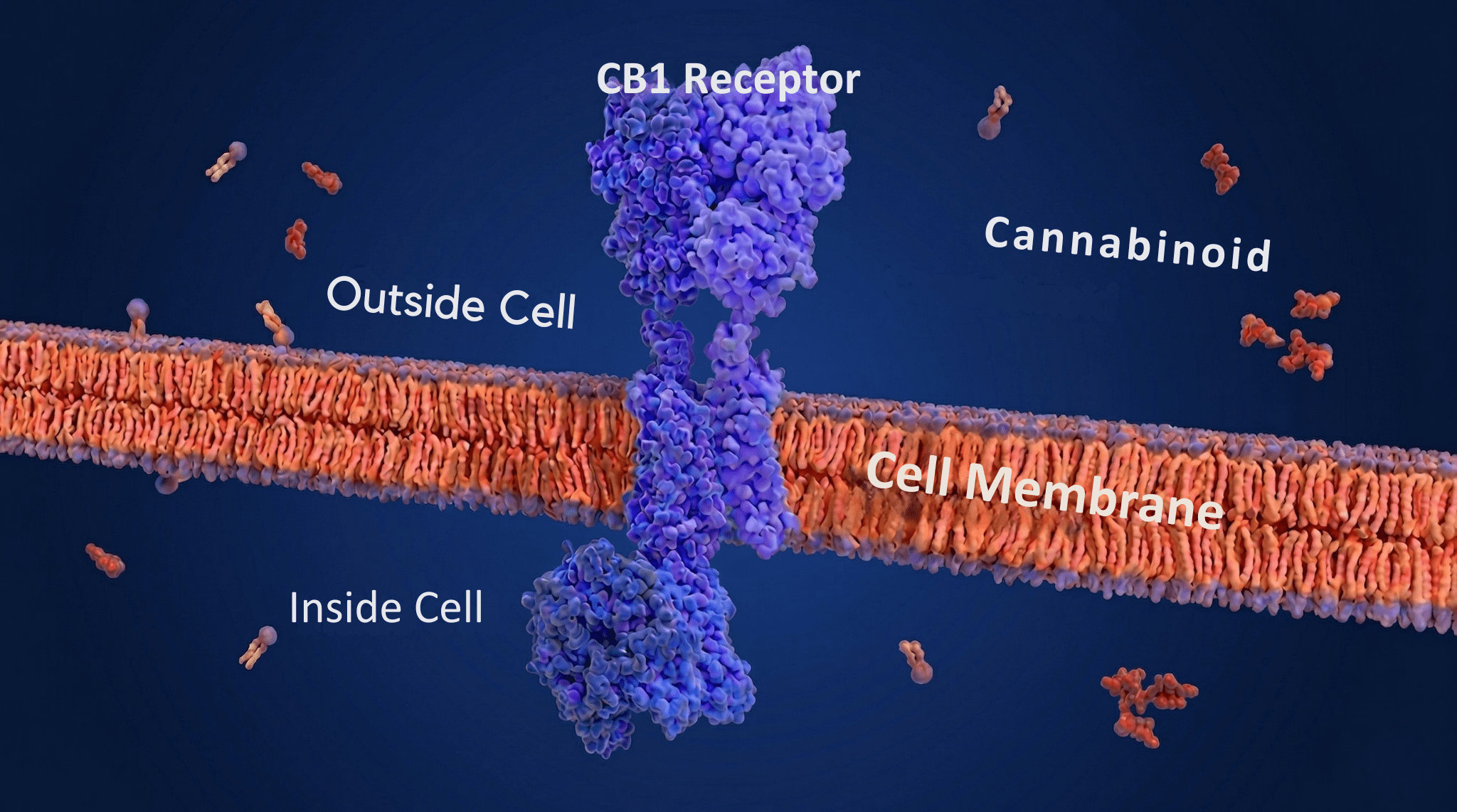
Cannabis affects sleep through its plant-based compounds—cannabinoids and terpenes—and the way they interact with the endocannabinoid system (ECS), your body’s built-in network of receptors and chemical signals that help regulate sleep, mood, and stress. Your brain and body already produce their own cannabinoids. One of the most important is anandamide, which binds to CB1 receptors—the brain’s primary docking sites for cannabinoids—in areas that control sleep, including the hypothalamus and basal forebrain (two brain regions that manage sleep timing and hormone release). There, it works with calming chemical systems (GABA and adenosine) to promote drowsiness (Murillo-Rodríguez et al., 2011). When external cannabinoids like THC and CBD enter the picture, the effects aren’t simply sedating: THC shortens the time it takes to fall asleep but also changes the structure of your sleep, which can affect memory and emotional processing (Nicholson et al., 2004).Why Cannabis Affects Everyone Differently
Cannabis doesn’t work the same way for everyone. Your tolerance—how accustomed your brain has become to a substance and how much more it now needs to feel the same effect—your history of use, genetic differences in the enzymes that process cannabinoids, and hormone-related biology all influence whether cannabis helps or hurts your sleep (Lowe et al., 2021). Even the terpenes—the aromatic compounds that give each strain its smell—play a role: myrcene and linalool may add to the sedating effect, while limonene and pinene can be alerting, creating competing effects within the same strain (Russo, 2011). Many people use cannabis specifically for insomnia (persistent trouble falling or staying asleep) tied to chronic pain, anxiety, or PTSD. In those cases, for many of these people, better sleep may come from relieving the underlying condition rather than from any direct change to sleep structure (Walsh et al., 2021). That said, regular heavy use—especially of high-THC products—can lead to tolerance, dependence (a state where the body relies on a substance to feel normal), and sleep problems when trying to cut back or stop (Budney et al., 2004).The Endocannabinoid System and Sleep
The ECS is a signaling system in the brain and body that helps regulate your internal balance—including sleep cycles, circadian rhythms (your body’s internal 24-hour clock), and energy. It has three main parts:- Your body’s own cannabinoids—primarily anandamide and 2-arachidonoylglycerol (2-AG)
- Cannabinoid receptors, mainly CB1 and CB2, found throughout the brain and body
- Enzymes that build and break down those cannabinoids (Mechoulam & Parker, 2013)
CB1 Receptors and Sleep
CB1 receptors are spread throughout the brain areas that control sleep—including the hypothalamus, basal forebrain, and brainstem (Lutz et al., 2015). They regulate the release of chemical messengers, particularly GABA (which slows brain activity) and glutamate (which excites it), directly affecting how awake or drowsy you feel (Murillo-Rodríguez et al., 2008). In animal studies, activating CB1 receptors increased NREM sleep—the deep, dreamless stages—and shortened the time needed to fall asleep, findings that have been partially confirmed in human studies using THC (Pava et al., 2016; Nicholson et al., 2004). When researchers blocked these same CB1 receptors in animal studies, sleep became fragmented and dream sleep shortened—showing that these receptors work in both directions, either promoting or disrupting healthy sleep depending on whether they’re activated or blocked (Pava et al., 2016). Using THC regularly over time causes the brain to dial back its CB1 receptors—reducing their number and making them less sensitive to stimulation. This is why tolerance develops: you need more THC to get the same effect, and over time, sleep quality can actually worsen as a result (Lutz et al., 2015).Daily ECS Rhythms
The ECS follows its own daily rhythm. Anandamide levels tend to rise during the early morning hours—the time humans are typically asleep—suggesting it plays a role in helping sleep begin (Murillo-Rodríguez et al., 2006). 2-AG levels peak later in the day, potentially supporting wakefulness and energy balance (Vaughn et al., 2010).How CBD Works Differently
CBD doesn’t bind strongly to CB1 or CB2 receptors. Instead, it targets receptors involved in mood, pain, and relaxation—including serotonin receptors, TRPV1 channels, and adenosine receptors—in ways that promote calm and may indirectly support sleep, especially in people whose insomnia is driven by anxiety (Russo, 2011; Shannon et al., 2019). The relationship between sleep and the ECS runs both ways. Disrupted sleep can also throw the ECS off balance—and altered ECS function has been found in people with chronic insomnia, sleep apnea (a condition where breathing repeatedly stops during sleep), and PTSD. This suggests cannabis-based therapies might work by targeting the brain processes already involved in these conditions (Babson et al., 2017).What THC, CBD, and CBN Do to Your Sleep
THC: Faster to Sleep, Less Dreaming
Sleep moves through two main stages: NREM sleep—the deep, restorative phases—and REM sleep, the stage when you dream, store memories, and process emotions (Carskadon & Dement, 2011). THC shortens how long it takes to fall asleep but also consistently reduces time spent in REM sleep (Cousens & DiMascio, 1973; Schierenbeck et al., 2008). For people with PTSD, that reduction in dream sleep can mean fewer nightmares (Fraser, 2009). But over time, suppressing REM may impair memory and emotional regulation (Walker, 2009).CBD: A Two-Phase Effect
CBD behaves differently depending on the dose—small amounts can be alerting, while larger amounts tend to be sedating. In animal studies, low-to-moderate doses activated brain systems involved in wakefulness, suggesting potential for treating daytime sleepiness, though human trial evidence for this remains limited (Murillo-Rodríguez et al., 2008; Chagas et al., 2014). At higher doses, CBD has been shown to increase total sleep time and deepen sleep in human case series (detailed reports on results from a group of real patients) (Shannon et al., 2019). In practical terms: lower doses earlier in the day may help you stay alert, while higher doses in the evening may help you sleep.CBN and the Entourage Effect
CBN—a compound produced as THC breaks down over time—has attracted interest as a sleep aid. Early research and anecdotal reports suggest it may extend total sleep time without suppressing dream sleep. But rigorous human studies are limited, and because CBN is almost always consumed alongside leftover THC and other cannabinoids, figuring out what CBN does on its own is genuinely difficult (Russo, 2011). This gets into what’s called the entourage effect—the idea that cannabinoids, terpenes, and other plant compounds work better together than any one of them does alone. Myrcene may boost the sleep-promoting properties of THC or CBN (Russo, 2011), while linalool has shown sedating effects in animal studies (Linck et al., 2009). A well-matched ratio of THC and CBD with the right terpenes may offer better results than any single compound alone.Cannabis and REM Sleep
Reducing REM sleep is one of the most consistent effects of cannabis documented in research. Studies going back to the 1970s found that moderate-to-high THC doses cut the proportion of time spent in dream sleep while increasing slow-wave (deep) sleep (Cousens & DiMascio, 1973; Feinberg et al., 1975). This happens because THC activates CB1 receptors in the brainstem—the part of the brain that controls wakefulness and triggers dream sleep. That activation disrupts the brain chemicals that normally switch REM sleep on, including serotonin and norepinephrine (two chemicals that regulate mood and arousal), delaying REM and cutting it short (Murillo-Rodríguez et al., 2008). The relationship runs both ways. When people who use cannabis nightly reduce or stop, many experience a REM rebound—a temporary surge of intense, vivid dreaming that can be jarring (Feinberg et al., 1976; Schierenbeck et al., 2008). CBD, by contrast, may modestly increase REM sleep at moderate doses through its anti-anxiety and serotonin-related effects (Babson et al., 2017). How much any of this matters in practice depends on the cannabinoid mix, dose, product type, and how often someone uses (Babson et al., 2017; Suraev et al., 2020).Cannabis and Your Body Clock
The ECS follows its own daily rhythm: anandamide and 2-AG levels rise and fall throughout the day in sync with waking, eating, and sleep (Valenti et al., 2004; Murillo-Rodríguez et al., 2006). When THC or CBD is introduced, it can shift these rhythms by changing how active the ECS is at different points in the day. Timing matters. High-THC cannabis used late in the evening may help you fall asleep faster (Nicholson et al., 2004). High-CBD products used earlier in the day may reduce anxiety and nervous system over-activity in ways that could support a more stable sleep-wake cycle—though this comes from CBD’s documented anti-anxiety effects (Shannon et al., 2019) rather than from dedicated circadian studies. For people with a disrupted body clock—from shift work or jet lag—cannabis might work alongside behavioral strategies. Animal studies show that activating cannabinoid receptors can influence how the brain adjusts to changes in light and darkness, possibly through the suprachiasmatic nucleus (SCN)—the brain’s master clock, located in the hypothalamus (Acuna-Goycolea et al., 2010). The same product may hit differently depending on whether you use it in the morning, afternoon, or evening, which suggests that timing is a real variable that hasn’t been studied enough. Heavy or long-term THC use at night may reduce deep sleep quality and leave you groggy the next day (Feinberg et al., 1975; Schierenbeck et al., 2008). For regular users, strain, dose, and timing all deserve deliberate thought.Cannabis Tolerance, Withdrawal, and Sleep Disruption
Short-term cannabis use often helps with sleep onset. But long-term use leads to tolerance and, in many cases, rebound insomnia—a temporary worsening of sleep when you stop. Over time, the brain adapts to regular THC by reducing the sensitivity of its CB1 receptors, meaning you need more to get the same effect, and sleep quality can actually decline in the process (Lutz et al., 2015). When long-term users stop abruptly, withdrawal commonly includes vivid dreams, difficulty falling asleep, and frequent waking. This happens because the brain overcorrects—the chemical systems that THC had been holding in check, including serotonin and norepinephrine signals, fire more strongly than usual. REM sleep, which had been suppressed, comes rushing back, often as intense or unsettling dreams. These disturbances can last several weeks (Budney et al., 2004). Tapering down gradually is a better approach than quitting suddenly. CBD, which is generally not habit-forming, may ease some withdrawal-related sleep problems through its calming and balance-restoring effects—though the research is still limited and results are mixed.Strategies for Cannabis-Related Sleep Issues
Not all cannabis-related sleep problems are the same. There’s a difference between primary insomnia (insomnia that isn’t caused by another condition), a sleep disorder triggered by cannabis itself, and sleep disruption caused by an underlying condition like anxiety or chronic pain. Sleep diaries, wearable trackers, and sleep studies can help figure out which is which. Cognitive Behavioral Therapy for Insomnia (CBT-I) is the most well-supported first-line treatment for chronic sleep issues and has been used with people tapering off cannabis. It works by identifying and changing unhelpful behaviors and thought patterns—like watching the clock or associating the bedroom with being awake—that can persist long after THC is out of your system. Medication is sometimes needed during early withdrawal, especially when the REM rebound causes significant distress. Sleep aids like zolpidem or antidepressants that also cause drowsiness, like trazodone, may be considered under medical supervision, though their own dependency risks need to be weighed carefully. Early evidence suggests CBD may reduce anxiety and calm the nervous system during this period, indirectly improving sleep, though results are mixed and dose-dependent (meaning effects vary with the amount taken). Lifestyle changes work alongside medication. Regular physical activity—especially in the morning or early afternoon—has been linked to deeper sleep and may help offset the tolerance to THC’s sedating effects that builds over time. Mindfulness-based stress reduction (MBSR) can lower physical tension that tends to run high during withdrawal. For people not ready to quit entirely, harm-reduction approaches—strategies focused on safer use rather than stopping completely—can limit the most disruptive effects: shifting use to earlier in the evening, lowering THC potency, or switching to balanced THC:CBD strains. Choosing strains high in myrcene or linalool—both of which have sedating properties in preclinical research (animal studies)—may allow users to reduce their THC load while preserving sleep-onset effects, though this hasn’t been tested directly in human sleep trials (Russo, 2011; Linck et al., 2009).What We Still Don’t Know About the Cannabis and Sleep
Most cannabis-sleep research is based on small samples, short-term studies, or recreational users rather than medical patients (Suraev et al., 2020). Long-term studies that follow people over time are needed to understand both the benefits and the risks—including what extended use of external cannabinoids does to the body’s own ECS over time. The dose-response relationship—how the effects of cannabis change as the amount used goes up or down—needs much more investigation. Low-to-moderate THC doses may shorten sleep onset, while higher doses appear to fragment dream sleep and cause next-day grogginess (Nicholson et al., 2004). CBD shows a two-phase pattern in animal studies—alerting at low doses, sedating at higher ones—but translating that into precise dosing guidelines for conditions like insomnia, REM sleep behavior disorder (a condition where people physically act out their dreams), or sleep apnea is one of the field’s biggest unanswered questions (Hsiao et al., 2012; Chagas et al., 2014). Older adults, women, neurodivergent individuals, and people with co-occurring mental health or chronic pain conditions may all respond differently to cannabinoids—but most studies have been done on young recreational users (Babson & Bonn-Miller, 2014). Genetic differences, like variation in how many cannabinoid receptors a person’s body produces, could affect both how well cannabis works and what side effects they experience, pointing toward personalized treatment as the right long-term framework. Research should also look at how cannabis interacts with established sleep treatments like CBT-I and chronotherapy (a treatment that uses scheduled sleep shifts and light timing to reset the body clock)—combining medication-based and behavioral approaches may offer the most lasting results for both medical and recreational users.Your Relationship with Cannabis and Sleep is Highly Individual
Cannabis’s relationship with sleep is not as simple as it makes people sleepy. THC and CBD interact with the ECS to affect the brain processes that control when you fall asleep, how long you sleep, and what your sleep looks like (Nicholson et al., 2004; Babson & Bonn-Miller, 2014). Under controlled conditions, cannabis shifts the balance of sleep stages—cutting dream sleep while extending deep sleep (Cousens & DiMascio, 1973; Feinberg et al., 1975). But that potential comes with real trade-offs: long-term or high-dose use can produce tolerance, diminishing returns, and disrupted sleep when you stop (Schierenbeck et al., 2008; Budney et al., 2004). How cannabis affects any individual also depends on how they process cannabinoids, their history of use, and whether they’re managing anxiety, PTSD, or chronic pain (Vandrey et al., 2011). Matching cannabinoid type, dose, and timing to each person’s biology and habits—including their circadian rhythms and any behavioral therapies they’re already using—is the most evidence-based approach available (MacCallum & Russo, 2018). Getting there will require rigorous, long-term, placebo-controlled studies (where some participants receive an inactive stand-in to allow fair comparison) that combine self-reported sleep quality with objective tools like polysomnography—overnight sleep monitoring—and wearable trackers, so cannabis sleep interventions can move from promising to genuinely proven.About the Author
RN Collins is a 1L at Northeastern University School of Law and a neuroscientist exploring how brain health and the environment intersect. Through her writing, she bridges academic research and science communication to reframe how psychoactive plants and other traditional and alternative medicines are understood. She’s building a career that connects law, technology, and creativity—and welcomes conversations and opportunities across fields that share that vision. Connect with her on LinkedIn!References
- Acuna-Goycolea, C., Obrietan, K., & van den Pol, A. N. (2010). Cannabinoids excite circadian clock neurons. Journal of Neuroscience, 30(30), 10061–10066. https://doi.org/10.1523/JNEUROSCI.5838-09.2010
- Babson, K. A., & Bonn-Miller, M. O. (2014). Sleep disturbances among veterans in residence at a Veterans Administration Mental Health Residential Rehabilitation Treatment Program. Journal of Clinical Sleep Medicine, 10(12), 1377–1382.
- Babson, K. A., Sottile, J., & Morabito, D. (2017). Cannabis, cannabinoids, and sleep: A review of the literature. Current Psychiatry Reports, 19(4), 23.
- Budney, A. J., et al. (2004). Review of the validity and significance of cannabis withdrawal syndrome. American Journal of Psychiatry, 161(11), 1967–1977.
- Carskadon, M. A., & Dement, W. C. (2011). Normal human sleep: An overview. In M. H. Kryger, T. Roth, & W. C. Dement (Eds.), Principles and Practice of Sleep Medicine (5th ed., pp. 16–26). Elsevier Saunders.
- Chagas, M. H., et al. (2014). Effects of acute systemic administration of cannabidiol on sleep-wake cycle in rats. Journal of Psychopharmacology, 27(3), 312–316.
- Cousens, K., & DiMascio, A. (1973). (-)delta-9-Tetrahydrocannabinol as a hypnotic: An experimental study of three dose levels. Psychopharmacologia, 33(4), 355–364.
- Feinberg, I., et al. (1975). Effects of high dosage delta-9-tetrahydrocannabinol on sleep patterns in man. Clinical Pharmacology & Therapeutics, 17(4), 458–466.
- Feinberg, I., et al. (1976). Delta-9-tetrahydrocannabinol and natural sleep. Archives of General Psychiatry, 33(9), 1107–1111.
- Fraser, G. A. (2009). The use of a synthetic cannabinoid in the management of treatment-resistant nightmares in posttraumatic stress disorder (PTSD). CNS Neuroscience & Therapeutics, 15(1), 84–88.
- Hsiao, Y. T., et al. (2012). Effect of cannabidiol on sleep disruption induced by the repeated combination tests consisting of open field and elevated plus-maze in rats. Neuropharmacology, 62(1), 373–384.
- Linck, V. M., et al. (2009). Inhaled linalool-induced sedation in mice. Phytomedicine, 16(4), 303–307.
- Lowe, D. J. E., et al. (2021). Cannabis and mental health: Putting the record straight. Addiction, 116(11), 2975–2980.
- Lutz, B., et al. (2015). The endocannabinoid system in guarding against fear, anxiety and stress. Nature Reviews Neuroscience, 16(12), 705–718.
- MacCallum, C. A., & Russo, E. B. (2018). Practical considerations in medical cannabis administration and dosing. European Journal of Internal Medicine, 49, 12–19.
- Mechoulam, R., & Parker, L. A. (2013). The endocannabinoid system and the brain. Annual Review of Psychology, 64, 21–47.
- Murillo-Rodríguez, E., et al. (2006). Anandamide enhances extracellular levels of adenosine and induces sleep: An in vivo microdialysis study. Sleep, 29(2), 178–185.
- Murillo-Rodríguez, E., et al. (2008). The endocannabinoid system modulating levels of consciousness, emotions and likely dream contents. Journal of Neuroscience, 28(28), 7080–7089.
- Murillo-Rodríguez, E., et al. (2011). Anandamide and sleep-wake cycle. Progress in Neuro-Psychopharmacology and Biological Psychiatry, 35(2), 373–382.
- Nicholson, A. N., et al. (2004). Effect of delta-9-tetrahydrocannabinol and cannabidiol on nocturnal sleep and early-morning behavior in young adults. Journal of Clinical Psychopharmacology, 24(3), 305–313.
- Pava, M. J., et al. (2016). Endocannabinoid modulation of cortical up-states and NREM sleep. PLoS ONE, 11(2), e0149745.
- Russo, E. B. (2011). Taming THC: Potential cannabis synergy and phytocannabinoid-terpenoid entourage effects. British Journal of Pharmacology, 163(7), 1344–1364.
- Schierenbeck, T., et al. (2008). Effect of illicit recreational drugs upon sleep: Cocaine, ecstasy and marijuana. Sleep Medicine Reviews, 12(5), 381–389.
- Shannon, S., et al. (2019). Cannabidiol in anxiety and sleep: A large case series. The Permanente Journal, 23, 18–041.
- Suraev, A. S., et al. (2020). Cannabinoid therapies in the management of sleep disorders: A systematic review of preclinical and clinical studies. Sleep Medicine Reviews, 53, 101339.
- Valenti, M., et al. (2004). Differential diurnal variations of anandamide and 2-arachidonoyl-glycerol levels in rat brain. Cellular and Molecular Life Sciences, 61(7–8), 945–950.
- Vandrey, R., et al. (2011). A within-subject comparison of withdrawal symptoms during abstinence from cannabis, tobacco, and both substances. Drug and Alcohol Dependence, 92(1–3), 48–54.
- Vaughn, L. K., et al. (2010). Endocannabinoid signalling: Has it got rhythm? British Journal of Pharmacology, 160(3), 530–543.
- Walker, M. P. (2009). The role of sleep in cognition and emotion. Annals of the New York Academy of Sciences, 1156(1), 168–197.
- Walsh, J. H., et al. (2021). Treating insomnia symptoms with medicinal cannabis: A randomized, crossover trial of the cannabis flower. Sleep, 44(11), zsab149.